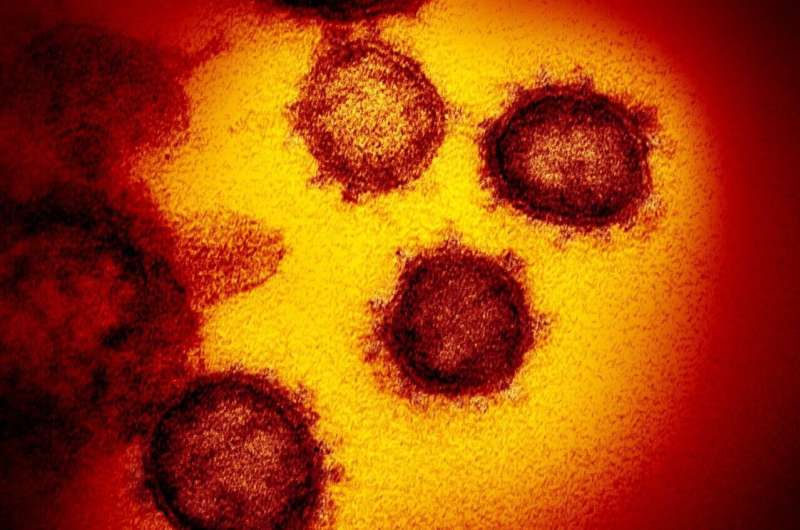
A preliminary study to be presented at this year’s European Congress of Clinical Microbiology & Infectious Diseases (ECCMID) in Lisbon, Portugal (23-26 April), suggests that people living with HIV who are on antiretroviral treatment (ART) with protease inhibitors (PI), may have a lower risk of COVID-19 infection. The study is by Dr. Steve Nguala from the Intercommunal Hospital Center of Villeneuve-Saint-Georges and the General Hospital of Melun in France and colleagues.
Despite these important findings, the authors underscore that it is a small, early, observational study and should not be taken as conclusive evidence that long-term use of protease inhibitors will protect people living with HIV from COVID-19.
People living with HIV are at greater risk of community or opportunistic infections, but they do not appear to be at increased risk for serious COVID-19, possibly because of their use of ART. Antiretroviral therapy was proposed as a protective factor against Severe Acute Respiratory Syndrome (SARS) in 2003, but the small number of cases did not permit conclusions to be drawn.
Protease inhibitors, a class of antiviral drugs used to treat HIV, work by blocking a critical enzyme (called a protease) that viruses need to replicate and infect more cells. While they have not been shown to cure COVID-19 infections in the general population, their efficacy to prevent COVID-19 is unknown.
To explore this further, Nguala and colleagues conducted a multicentre cohort study in six hospitals in Ile-de-France to assess the impact of long-term use of PI in patients with HIV on the incidence of COVID-19. Between May 1, 2020, and May 31, 2021, they enrolled 169 people with HIV who were been treated with ART with PI, and 338 patients with HIV taking ART without PI. None of the participants had been previously been diagnosed with COVID-19, the average age was 50 years (48% female; 52% male).
Among participants being treated with PIs, over three-quarters were taking darunavir/ritonavir (131/169; 77%), around 8% were taking atazanavir/ritonavir (14/169), and the rest were treated with other PIs (24/169;14%). On average, they had been taking PIs for at least a year.
All patients had regular clinical assessments and screening for COVID-19 during the usual HIV follow-up (every 6 months). Modelling was performed to identify potential risk factors associated with COVID-19.
Over a year of follow-up (with some patients lost to follow-up in both groups) 12% (18/153) of participants taking PIs and 22% (61/283) of those in the non-PI group contracted COVID-19 assessed by positive SARS-COV-2 serology at the end of study; and four patients in the non-PI group were admitted to hospital with COVID-19.
After adjusting for factors that are linked with increased risk of COVID-19 including gender, age, CD4 cell count, number of people living in the household, contact with a positive COVID-19 case, the researchers found that patients in the protease inhibitor group were 70% less likely to become infected with COVID-19 compared to those in the non-PI group.
Patients in both groups who had been in contact with COVID-19 in the 14 days prior to their consultation were twice as likely to test positive for COVID-19; while those living in the same household with at least three other people were three times as likely to test positive; and those who had lost their sense of taste were six times as likely to be diagnosed with COVID-19 (see table in notes to editors).
“Protease inhibitor drugs have long history of use, a good safety profile, and are generally well tolerated. By attacking the virus before it has a chance to multiply they potentially offer an opportunity to prevent the spread of infections and mutation of future variants”, says Dr. Nguala. “The lower occurrence of COVID-19 among patients treated with a protease inhibitor-based regimen raises the question of a preventive effect that should be further investigated. More studies with a larger number of patients, and in randomised trials in people without HIV, are needed to confirm these preliminary results. The challenge will be to produce robust data in a limited period that may inspire new prevention or therapeutic strategies.”
European Society of Clinical Microbiology and Infectious Diseases

